What to Do for your Pre-Op Physical: Be Ready for Surgery


Imagine walking into the operating room feeling confident that you’re well-prepared for your upcoming surgery. This level of confidence stems from a thorough preoperative evaluation, which includes a detailed pre-assessment to evaluate your health, medical history, and home circumstances. A comprehensive pre-op assessment is the foundation of a smooth surgical experience and a speedy recovery.
In this blog post, we will take you on a journey through the various aspects of pre-op evaluation, from understanding the essentials to managing perioperative risks. Discover the importance of medical history, cardiac and pulmonary examinations, and the role of prehabilitation which optimizes your health before surgery to deal with potential health issues in the recovery period. Let’s get started!
For a practical checklist and step-by-step guidance on preparing for surgery, explore this complementary guide.
Key Takeaways
Pre-op procedures are necessary to assess a patient’s overall health and identify potential risks.
Comprehensive medical history, physical exam including cardiac and pulmonary evaluation, tailored pre-op tests provide an overview of health status prior to surgery. Attending a pre assessment appointment is crucial as it involves a nurse-led clinic appointment to check the patient's health, medical history, and home circumstances, and conduct various tests such as blood tests, ECG, MRSA screen, weight, height, and blood pressure checks.
Prehabilitation programs work to support patients before and after surgery with tools such as nutritional supplementation, medications, exercise and stress management.
If you are unsure about any step throughout the process, learn more about some of the top questions to ask before surgery.
What to Do for a Pre-Op Physical: Key Steps to Prepare
Understanding what to do for a pre-op physical is essential for a safe surgery. During your pre-op appointment, doctors evaluate your heart, lungs, and medical history to detect any risks. Spotting conditions like vascular disease or respiratory issues early helps create a safer surgical plan and speeds up recovery.
The patient’s medical history is the main element of preoperative evaluation. It helps identify potential risks and complications such as allergies, prior reactions to anesthesia, and existing health conditions like coronary artery disease. The pre-op physical exam is another essential aspect of the evaluation, where physicians assess the patient’s heart, lungs, and overall health. Blood tests are often part of the pre-op evaluation to assess the patient's health status. This extensive evaluation aids in customizing the pre-op assessment to the patient’s specific needs, promoting the best surgical outcomes.
The Role of Medical History in Pre-Op Assessment

An extensive medical history offers important information that can greatly influence the preoperative evaluation process. The patient’s medical record includes:
Past and current medical history
Surgical history
Family history
Social history
History of allergies
Current and recent drug therapy
Unusual reactions or responses to drugs
Any problems or complications associated with previous anesthesia
For example, it is crucial to carefully assess diabetic patients for potential complications and ensure proper blood glucose control preoperatively and postoperatively.
Such information helps healthcare practitioners get an overview of a patient’s medical status in order to provide better care, such as allowing healthcare providers to assess the potential risk of pulmonary complication rates ranging from mild to severe.
In addition to a thorough history, a clinical examination is also crucial in determining the presence of a disease. Routine laboratory tests, however, may not present a benefit or cost-effectiveness for apparently healthy patients. Merging medical history with physical examination allows healthcare providers to better recognize patients with a higher risk for perioperative complications and make well-founded decisions about their anesthesia and surgical care.
Physical Exam: A Closer Look at Your Health
During the pre-op physical examination, healthcare providers evaluate the patient’s airway, lungs, and heart, along with recording vital signs. This comprehensive physical examination helps identify potential cardiac and pulmonary complications and ascertain the patient’s functional heart and lung capacity. These evaluations are often conducted in a pre-assessment clinic to ensure comprehensive health checks.
We'll discuss in more detail the cardiac and pulmonary evaluations and their importance in pre-op assessment.
Cardiac Evaluation
Evaluating potential cardiovascular risk, including the presence of cardiovascular disease, is necessary to assess the patient’s ability to withstand surgery and anesthesia. Perioperative cardiovascular evaluation plays a crucial role in identifying potential cardiac events, including myocardial infarction, pulmonary edema, ventricular and atrial fibrillation, primary cardiac arrest, and complete heart block, which can have a major impact on the results of a surgical procedure. Ignoring these issues can put the success or failure of operations at risk. A comprehensive cardiac evaluation aids in recognizing these risks, which can be handled through suitable interventions like unblocking cardiac arteries with angioplasty, preventing the blood from dangerous clotting with use of non-steroidal meds like aspirin, and slowing the heart rate and lowering the blood pressure with beta-blockade, and angiotensin-converting enzyme inhibitor therapy.
A cardiac evaluation typically involves a thorough history and physical examination, focusing on risk factors for cardiac complications. Additional tests such as cardiac stress tests or coronary computed tomography angiography (CCTA) which may be ordered based on the patient’s clinical history, comorbidities, and physical examination findings. This comprehensive cardiac assessment helps ensure that the patient is well-prepared for surgery and anesthesia.
Pulmonary Examination
Evaluating pulmonary function is crucial for identifying potential respiratory complications that may occur during surgery, and ensuring the patient’s lungs can handle the stress of surgery. During a pulmonary examination, physicians assess specific signs such as:
adventitious lung sounds - any sounds that are out of the ordinary
wheezing - whistling or rattling sound in the chest
rales - small bubbling, rattling or clicking sounds in the lungs
rhonchi - low-pitches noises made when exhaling
or other signs of active narrowing of the airway caused by spasm, infection, or tumor
Preoperative pulmonary function testing, including:
spirometry, which measures lung air capacity
diffusion capacity test, which measures how well the lungs exchange gases, and
arterial blood gas analysis, which measures the amount of gases dissolved in arterial blood
can also help assess the patient’s lung function and risk of complications.
Certain risk factors, such as chronic obstructive pulmonary disease, abdominal and thoracic surgery, and emergency surgery, may be associated with perioperative respiratory complications. Recognizing these risk factors and conducting a comprehensive pulmonary examination allows healthcare providers to plan perioperative interventions effectively and improve the patient’s respiratory health before surgery. As surgical and anesthesia complications appear to be more common in these cases, it is crucial to be vigilant and proactive in addressing them.
Pre-Op Testing: What to Expect

Pre-op tests are a key part of the preoperative evaluation process, aiding in securing the best possible outcomes for surgical patients. These tests are tailored to the individual patient’s medical history and needs, taking into account factors such as the type of surgery, anesthesia, and any underlying health conditions. Pre-op tests may include blood work, imaging studies, and other diagnostic tests to provide a comprehensive overview of the patient’s health status.
Attending a pre operative assessment appointment is crucial to complete necessary tests and evaluations, ensuring the patient is fit for surgery.
To avoid delays in surgery, patients should ensure that the physicians responsible for their pre-operative tests submit the results to their surgeon and anesthesiologist. Appropriate pre-op testing aids healthcare providers in making well-founded decisions about anesthesia and perioperative care, eventually resulting in better surgical outcomes and a quicker recovery. This is especially crucial for urgent and emergency procedures, where time is of the essence.
Special Considerations for Patients with Specific Conditions
Patients with certain conditions, such as diabetes, heart disease, or those taking anticoagulant medications, require thorough pre-operative management to reduce perioperative risks. For instance, patients on anticoagulant therapy should have their coagulation status optimized before undergoing regional anesthesia to avoid excessive bleeding.
In some cases, spinal anesthesia can be beneficial as it reduces postoperative mortality and morbidity. However, it is crucial to consider the risks and benefits, especially in patients on anticoagulant therapy, to ensure safe outcomes.
Corticosteroid-treated asthmatics, for example, may need to adjust their medication regimen prior to surgery to minimize the risk of perioperative complications. Consulting with healthcare providers is necessary to determine the required adjustments to medications and any special precautions needed before surgery.
Surgical Procedures and Anesthesia Types
The type of surgery and anesthesia used can impact perioperative risk, and should be considered during pre-op evaluation. For example, patients undergoing vascular surgery may require intraoperative anticoagulation with heparin; however, in combination with spinal surgery, this potentially might cause abnormal bleeding complications.
Keep in mind that certain medications taken for arthritis and pain like COX-1 & COX-2 inhibitors and NSAIDs, medicines to prevent platelets from sticking together like thienopyridines, and platelet glycoprotein (GP) IIb/IIIa antagonists, are known to increase the risk of bleeding during spinal/epidural anesthesia. Proper management of these medications and anesthesia techniques is crucial in minimizing perioperative risks.
The Day Before Surgery: Final Preparations

The day before surgery, patients should follow specific guidelines to ensure they are ready for the procedure. Here are some important steps to take:
Fasting is crucial to decrease the volume and acidity of stomach contents, reducing the likelihood of regurgitation and aspiration during surgery.
Typically, patients are advised not to consume any solid food for a certain period of time.
Clear liquids may be permitted up to a few hours before the surgery.
Any sudden change noted in the immediate pre-op period such as a fever, nausea, cough or “cold”-type symptoms should be immediately reported to the pre-op department where the planned operation is to take place.
It is also important to review the appointment letter for specific instructions and details about the surgery.
Besides fasting, patients may need to modify their medication intake before surgery. For example, abrupt discontinuation of drugs such as clonidine should be avoided to prevent rebound hypertension. Smoking cessation and abstaining from alcohol consumption for at least 24 hours before surgery are also recommended. By adhering to these guidelines, patients can optimize their physical and mental preparedness for surgery.
Getting Help
Seeking additional support and resources can help patients better prepare for surgery and optimize their recovery process. Prehabilitation programs, such as those focusing on exercise, nutrition, and stress management, can significantly improve post-surgical outcomes.
A pre assessment nurse plays a crucial role in providing information and instructions to ensure patient safety before and after surgery.
We'll further discuss the role of prehabilitation and useful resources for additional assistance.
The Role of Prehabilitation
Prehabilitation, or physical and emotional preparation before surgery, can have a noticeable impact on post-surgical outcomes and overall recovery. Research has shown that prehabilitation improves various outcome domains preoperatively, including:
Nutritional supplementation
Smoking cessation
Physical and cognitive exercise
Stress management
Patients can improve their physical status, reduce functional decline, and optimize their recovery process by participating in prehabilitation exercises such as:
Aerobic exercises
Resistance exercises
Flexibility exercises
Balance exercises
Strength exercises
Inspiratory muscle training
Psychological interventions may also prove beneficial in certain prehabilitation programs.
Valuable Resources for Additional Assistance
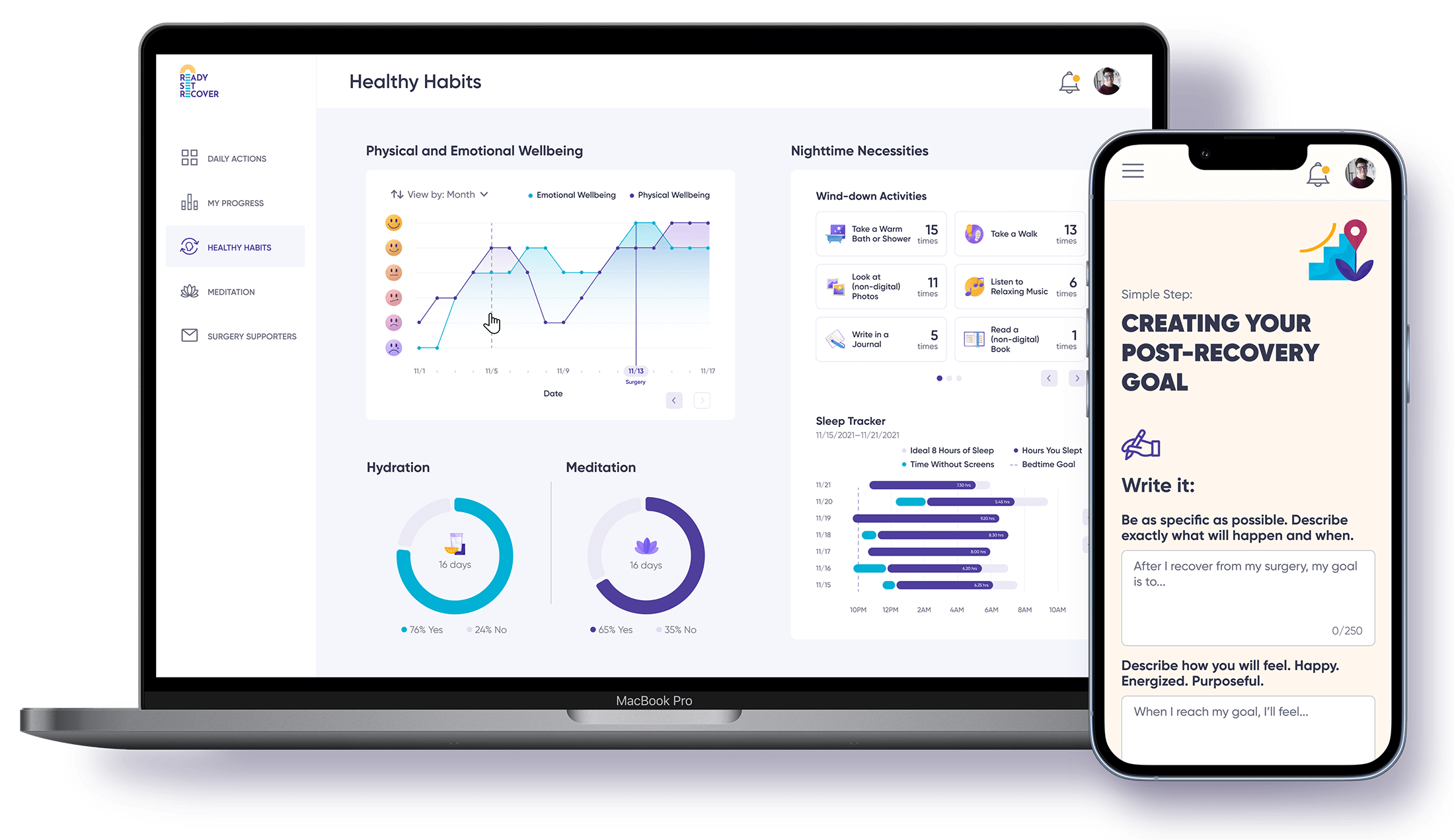
Programs like Ready Set Recover offer guidance and support for patients preparing for surgery. Covering topics such as sleep, stress management, and goal setting, this program aims to optimize recovery and overall well-being. Created by health and wellness professionals and approved by physicians,Ready Set Recover provides a comprehensive approach to pre-surgical preparation.
What to Do for a Pre-Op Physical: Final Prep for Surgery Success
In conclusion, a comprehensive pre-operative evaluation is crucial in ensuring a successful surgical outcome and a smooth recovery process. By understanding the essentials of pre-op assessment, taking into account medical history, and conducting thorough cardiac and pulmonary evaluations, patients and healthcare providers can work together to minimize perioperative risks.
By seeking additional support and resources, such as prehabilitation programs and organizations like Ready Set Recover, patients can take control of their pre-op journey and optimize their recovery process. With the right preparation and guidance, patients can face surgery with confidence, knowing they have taken every possible step to ensure the best possible outcome.
Frequently Asked Questions
What does pre-op mean?
Pre-op refers to the period before surgery, meaning "before operation." During this time, you will meet with doctors or representatives from surgery and anesthesia. Most patients also have a pre-op appointment within the month before surgery to review their health and ensure they are ready for the procedure
How long does pre-op take before surgery?
Pre-op may take up to 4 hours, so it is important to bring your packet and personal reading material for the duration of the appointments. A thorough pre-op assessment can help reduce the length of hospital stay by minimizing complications.
What is a pre-op order for surgery?
A pre-op order for surgery is a process involving a member of the surgery/anesthesia departments who obtains basic information about you and your health, and it may include pre-operative testing such as blood and urine tests.
What is pre-op vs post-op?
Pre-operative care involves preparing a patient for surgery, while post-operative care refers to the care patients receive after a surgical procedure.
How does medical history play a role in pre-op assessment?
A detailed medical history helps doctors spot potential risks, such as allergies, past anesthesia reactions, or existing conditions. Understanding what to do for a pre-op physical ensures a smooth evaluation, helping doctors create the safest surgical plan for you.